
Written by Dr. Diane Mueller
Are at-home Lyme disease tests accurate? Usually, not enough to rule Lyme in or rule it out on their own.
That answer frustrates people for a reason. You do the responsible thing. You order the kit, prick your finger, mail it in, and wait for clarity. Then the result comes back negative while your body still says something is wrong, fatigue, head pressure, migrating joint pain, brain fog, air hunger, numb hands at 2 a.m. I’ve seen that pattern again and again in people from Greenwich to Stamford, and I’ve lived close enough to this kind of illness to know how fast doubt can creep in.
The core issue is simple: most at-home Lyme kits look for your immune response, not the bacteria itself. If your body has not made enough antibodies yet, or if your immune system is worn down, the test can miss it. This article explains how these tests work, how accurate they really are, where they help, and when you need a full clinical evaluation instead.
At-home Lyme disease tests are not accurate enough to rule Lyme disease in or out on their own because most rely on antibody detection with significant blind spots.
Testing too early can cause false negatives, since Lyme antibodies often take 2 to 6 weeks to rise after a tick bite or symptom onset.
A negative home result does not reliably exclude Lyme disease, especially in early infection, after recent antibiotics, or when immune response is impaired.
At-home kits can serve as a first screening step, but they cannot confirm active infection, identify co-infections, or explain overlapping issues like mold exposure or thyroid problems.
If your symptoms and exposure history still suggest Lyme disease, get a full clinical evaluation instead of relying on another at-home test.
Track your bite date, symptoms, and exposures before testing so a clinician can interpret any Lyme disease test in the right clinical context.
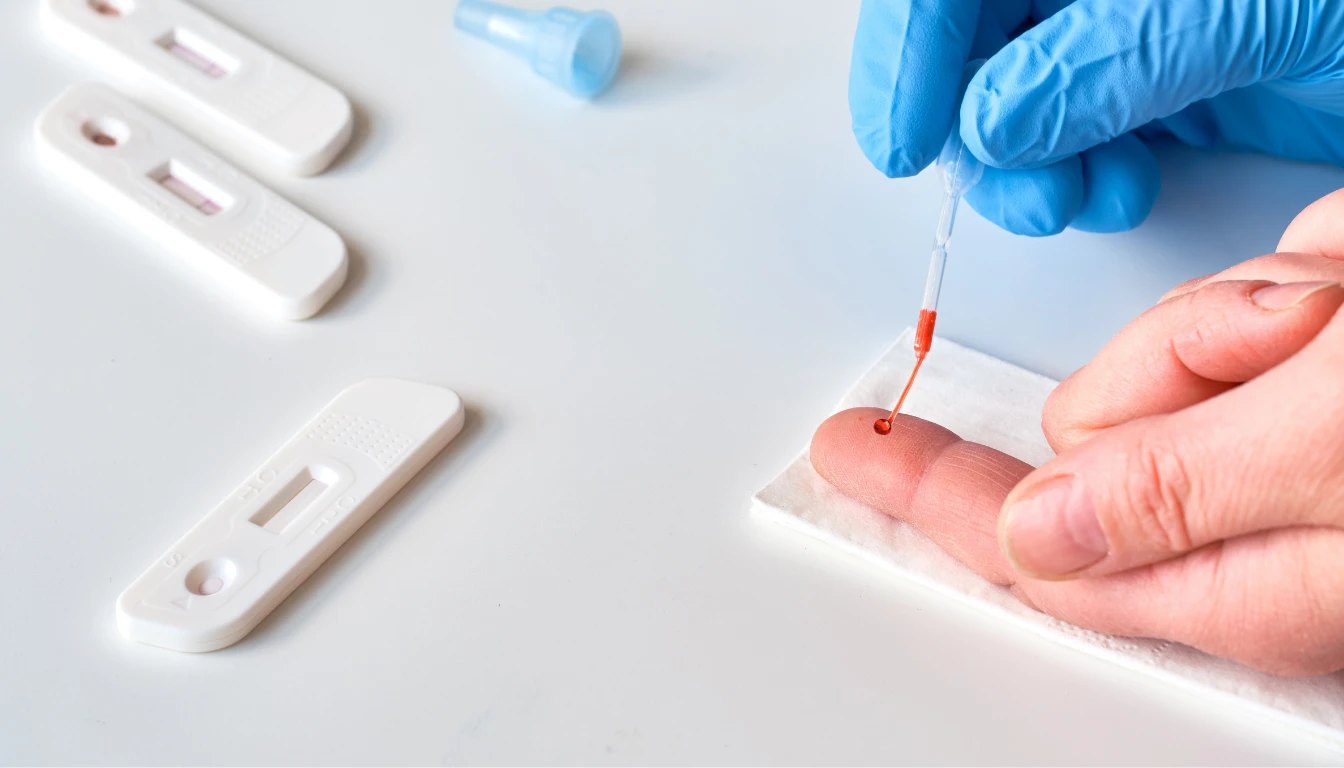
Most at-home Lyme kits use the same basic lab logic as standard office-based blood tests. They collect a small blood sample, then look for antibodies linked to Borrelia burgdorferi, the main Lyme bacteria identified in the U.S.
You are not usually testing for live bacteria. You are testing for signs that your immune system reacted to exposure. That difference matters.
The most common method is standard two-tier testing. This usually means:
An ELISA or similar screening test first
A Western blot or second immunoblot test if the first test is positive or unclear
Measurement of IgM and IgG antibodies
This is the approach long recommended in mainstream practice. But it has a known weakness: sensitivity can be poor, especially early on. Some reviews place standard two-tier sensitivity around 53.7% overall, with much worse performance in early infection.
If you want a plain-English comparison of home kits versus other options, this guide on choosing a Lyme disease test kit for your situation can help sort the categories.
There are also newer direct-detection methods under study or limited clinical use. These may look for bacterial DNA or other markers. But those are not what most at-home kits offer.
Action step: Check the kit description before you buy. If it only measures antibodies, do not treat a negative result as a final answer. Spend 5 minutes reading the method page first.
Here is the blunt truth. Most at-home kits can measure antibodies. They cannot confirm active infection.
They also usually cannot tell you:
Whether the infection is old or current
Whether symptoms come from Lyme alone or from co-infections
Whether treatment is working
Whether another Borrelia species is involved
Whether mold illness, autoimmunity, thyroid issues, or gut dysfunction are also driving symptoms
That last point is where many people get stuck. A person may have Lyme exposure, mold exposure, nervous system dysfunction, and hormone disruption at the same time. One mail-in test will not sort that out.
For a broader breakdown of test choices, this overview of Lyme disease tests explains why one result rarely tells the whole story. And if you want a general medical reference point, WebMD gives a useful high-level summary of how Lyme testing is commonly approached.
Action step: Write down your top 5 symptoms and your exposure history before you order any kit. That list often matters more than the report itself.
We have helped thousands of people in Colorado, Wyoming, New Jersey, Pennsylvania, Texas, Wisconsin restore their health and quality of life by diagnosing and treating their Lyme Disease.
Here is the short answer: at-home Lyme disease tests are usually only as accurate as the standard lab methods they rely on, and those methods have major blind spots.
Published data show a wide sensitivity range, roughly 7.4% to 86.2%, with an average near 59.5% depending on stage, method, and study design. In early Lyme, false-negative rates are often cited around 30% to 50%. That is not a small margin of error. That is a real risk of missed disease.
So if you are asking whether at-home Lyme disease tests are accurate enough to give peace of mind, the answer is often no. A negative home test can still happen in someone with real Lyme.
False negatives happen for several clear reasons.
Testing too early: antibodies may not be high enough yet
Recent antibiotics: early treatment can blunt antibody production
Immune suppression: some people simply do not mount a strong response
Collection issues: finger-prick samples can be harder to collect cleanly at home
False positives can happen too.
Cross-reactivity with other infections or immune activity
Non-standard interpretation criteria in some specialty labs
Past exposure without active illness now
I’ve seen both errors create damage. One patient delayed treatment because a home test came back negative three weeks after a tick bite. Another clung to a weak positive from a poorly validated panel while her main issue was severe mold exposure in a damp basement apartment near New Haven Harbor.
If you have a negative result but the story still fits, read this breakdown on false negative Lyme test. It explains the false-negative problem in practical terms.
Action step: If your result does not match your symptoms, do not stop there. Book a clinician review within 1 week and bring the full report.
Timing changes everything. Lyme antibody tests work best weeks after exposure, not right away.
In many cases, antibodies rise over 2 to 6 weeks. So the test window matters. Test on day 4 after a bite, and the result may be falsely reassuring. Test much later, and you may detect antibodies but still not know whether the infection is active.
Immune response matters too. People with long-term illness, mold exposure, chronic stress, poor sleep, or immune dysfunction may not produce predictable antibody levels. That means two people with similar infections can get very different results.
And the test method matters because many Lyme tests were built more for surveillance and standardization than for capturing every real-world case. For background on how medical evidence is organized and reviewed, the National Library of Medicine is a strong authority source.
If you are comparing options, this guide to the best Lyme disease test based on timing and symptoms is worth reading before you spend more money.
Action step: Put the date of your bite, rash, or first symptom on paper. Then compare that date to when you tested. That single step can change how you interpret the result.
We have helped thousands of people in Colorado, Wyoming, New Jersey, Pennsylvania, Texas, Wisconsin restore their health and quality of life by diagnosing and treating their Lyme Disease.
The biggest limitation is simple: an at-home Lyme test gives data, not a diagnosis.
That may sound obvious, but when you feel awful, any lab result can feel bigger than it is. People often give one test too much authority. Lyme does not work that neatly.
In early infection, the main problem is missing the case. Antibodies may not be there yet, which is why false negatives are so common in the first days and weeks.
In chronic or complex illness, the problem shifts. Now you may be dealing with:
old exposure plus current symptoms
immune exhaustion
previous antibiotic use
fluctuating antibodies
co-infections such as Babesia or Bartonella
mold-related inflammation that overlaps with Lyme symptoms
This is where people get told, “Your test is negative, so it can’t be Lyme.” That is often too simplistic. It is one reason Lyme disease misdiagnosis often happens.
I’ve watched patients carry years of labels, anxiety, fibromyalgia, chronic fatigue, IBS, before anyone looked at the full timeline. Sometimes the clue was a summer camping trip in Connecticut. Sometimes it was a “weird flu” after yard work near wooded trails in Fairfield County.
Action step: Build a one-page health timeline today. Include tick exposure, travel, mold exposure, onset of symptoms, and past treatments. It takes 20 minutes and helps far more than most people expect.
Lyme is often a clinical diagnosis, not a pure lab diagnosis. Symptoms, exposure history, physical findings, response patterns, and competing root causes all matter.
A single result cannot answer questions like these:
Is this Lyme, a co-infection, mold illness, or all three?
Is the nervous system stuck in fight-or-flight?
Is gut dysfunction blocking recovery?
Are thyroid or hormone issues adding fuel to the fire?
Sequence matters. If you treat one layer while missing another, progress stalls. That is why smart Lyme care often looks at the whole system instead of chasing one lab marker.
Action step: Stop asking only, “Was my Lyme test positive?” Start asking, “What full pattern explains my symptoms?” That question leads to better care.
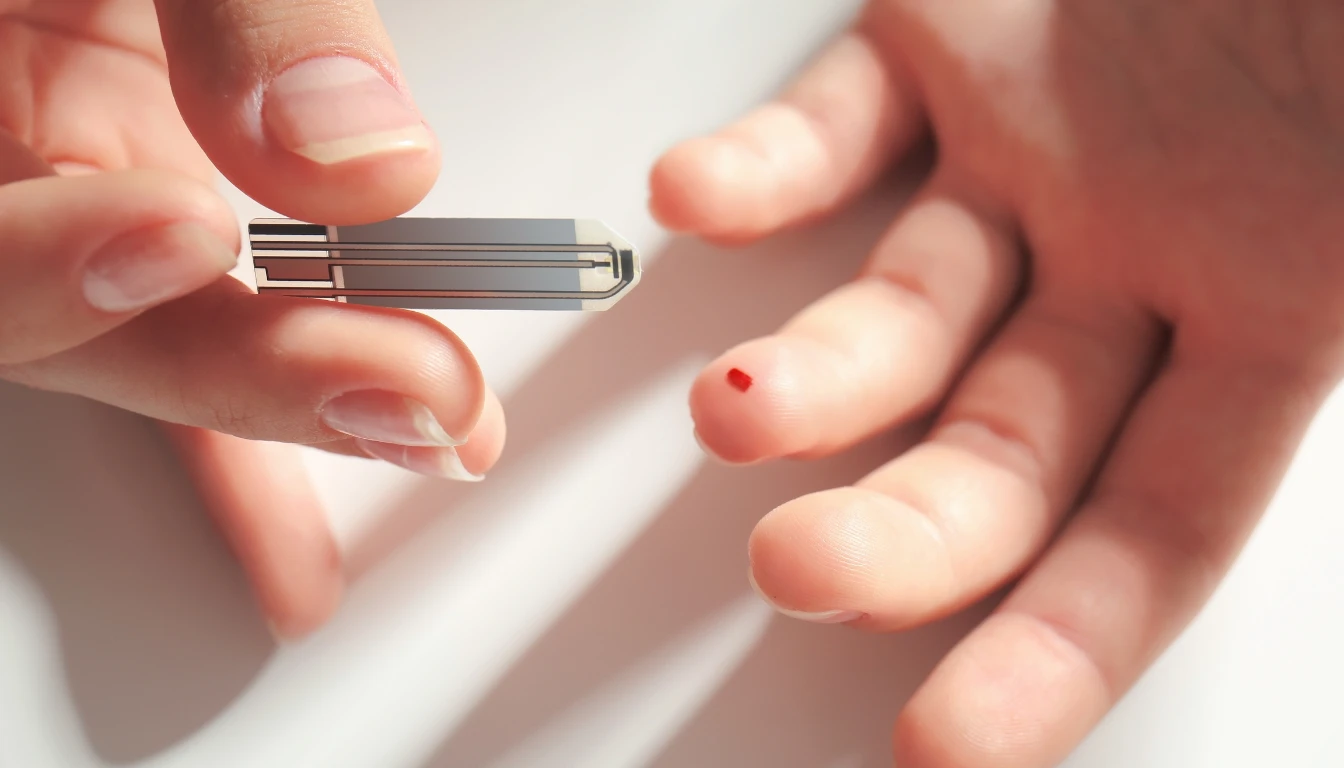
An at-home Lyme test can be helpful as a first screen, not as the final word.
It may make sense if you have mild symptoms, a known tick exposure, or limited access to care this week. It can also help if you want a documented result to bring to a clinician. In that role, home testing has some value.
It is most useful when all three are true:
your symptoms started after a possible exposure
you understand the kit’s limits
you plan follow-up either way
A positive result can support the case for urgent medical review. A negative result can still be useful if it pushes you to retest later or seek a deeper workup based on symptoms.
If you are trying to sort through which home kit is worth your money, this guide to choosing a Lyme disease test kit can save you from buying the first flashy ad you see.
Who this is for: people in the very early question stage who need a starting point. Who this is not for: people with months or years of neurological, hormonal, gut, fatigue, or multi-system symptoms.
Action step: Use a home test only if you also set a next step now. Decide today whether you will retest, see a doctor, or seek a full review if the result is unclear.
We have helped thousands of people in Colorado, Wyoming, New Jersey, Pennsylvania, Texas, Wisconsin restore their health and quality of life by diagnosing and treating their Lyme Disease.
If you have symptoms, a full clinical evaluation is often the better move. Do not rely on an at-home test alone if your body is clearly signaling that something is wrong.
You should get a full evaluation if you have:
fever, chills, or a bull’s-eye rash after a bite
joint pain, nerve pain, or facial droop
crushing fatigue or post-exertional crashes
brain fog, word-finding trouble, or memory lapses
air hunger, night sweats, palpitations, or dizziness
symptoms that have lasted more than a few weeks
a negative test that does not fit the clinical picture
This matters even more in places like Connecticut, where wooded exposure is common and many patients spend months being told their labs are “fine.” In my experience, the longer the illness has gone on, the less helpful a simplistic yes-or-no test becomes.
A full evaluation should review symptom history, exposure history, co-infections, mold risk, immune status, and other systems that affect recovery. That is how you stop guessing.
Action step: If you have 3 or more ongoing symptoms across different body systems, schedule a comprehensive visit instead of buying another home kit. Do it this week.
Before you trust any Lyme test, ask a few hard questions. The quality of the interpretation matters as much as the result itself.
Start here:
When did exposure happen? If it was recent, the test may be too early.
What method did the lab use? Was it standard two-tier testing or something else?
What exactly is being measured? Antibodies, DNA, or another marker?
Does the result match the symptom pattern? Labs should support the story, not erase it.
Could co-infections or mold illness be involved? A Lyme-only lens can miss the bigger picture.
Was the sample collected correctly? Home collection errors do happen.
What is the follow-up plan if the result is negative but symptoms continue?
One mistake I see often is blind trust in branding. A polished box does not equal a reliable test. Another is panic after an isolated positive from a lab with loose standards.
A better approach is simple: pair the lab with the timeline, symptoms, and clinical context.
Action step: Copy these seven questions into your phone notes before you order or review any Lyme test. Ask them at your next appointment. It takes 2 minutes.
At-home Lyme disease tests are not accurate enough to act as a stand-alone answer. They can be a starting point, but they often miss early infection, cannot confirm active disease, and do not explain the bigger picture in complex illness.
If your symptoms, exposure history, and instincts say something is off, trust that signal enough to keep going. The right next step is often not another random kit. It is a thorough clinical evaluation that looks at Lyme, co-infections, mold, immune function, and the sequence of what your body needs next.
Start here today: gather your symptom timeline, list your exposures, and bring every past test to a clinician who will look at the full pattern, not just one line on a lab report.
We have helped thousands of people in Colorado, Wyoming, New Jersey, Pennsylvania, Texas, Wisconsin restore their health and quality of life by diagnosing and treating their Lyme Disease.
Usually not. Most at-home Lyme disease tests rely on antibody testing, so they have the same limitations as standard lab tests. Early infection is often missed, with false-negative rates commonly cited around 30% to 50%, which means a negative result does not reliably rule out Lyme disease.
Most at-home kits use a finger-prick blood sample that is mailed to a lab for two-tier testing, typically an ELISA followed by a Western blot or immunoblot if needed. These tests look for IgM and IgG antibodies to Borrelia burgdorferi rather than detecting the live bacteria directly.
A negative result can happen if you test too early, take antibiotics before testing, or do not produce a strong antibody response. Because most home kits measure immune activity instead of the bacteria itself, symptoms and exposure history may matter more than one negative report.
No. Most at-home Lyme disease tests cannot confirm whether an infection is current, old, or fully active. They also usually do not identify co-infections like Babesia or Bartonella, and they cannot show whether another issue such as mold exposure or thyroid dysfunction is contributing to symptoms.
You should seek a full clinical evaluation if you have a bull’s-eye rash, fever, nerve symptoms, joint pain, severe fatigue, brain fog, or symptoms lasting more than a few weeks. A clinician can interpret testing alongside your history, timing of exposure, and overall symptom pattern.
Use it as a screening tool, not a final diagnosis. Check when your exposure happened, review whether the kit uses standard two-tier antibody testing, and make a follow-up plan before testing. If the result does not match your symptoms, schedule medical review rather than assuming the result is definitive.
Cook, M. J., & Puri, B. K. (2016). Commercial test kits for detection of Lyme borreliosis: A meta-analysis of test accuracy. International Journal of General Medicine, 9, 427–440. https://doi.org/10.2147/IJGM.S122313
Waddell, L. A., Greig, J., Mascarenhas, M., Harding, S., Lindsay, R., & Ogden, N. (2016). The accuracy of diagnostic tests for Lyme disease in humans, a systematic review and meta-analysis of North American research. PLoS ONE, 11(12), Article e0168613. https://doi.org/10.1371/journal.pone.0168613
We have helped thousands of
people restore their health
and quality of life by diagnosing
and treating their Lyme Disease.
“Dr. Mueller’s approach to medicine is refreshing! There is only so much you can do with western medicine and in my life I was needing a new approach. By addressing the whole body, nutritional diet factors, environmental factors, blood work, and incorporating ideas I had not previously known, I was able to break through with my conditions. I am not only experiencing less pain in my life, but through the process of healing guided by Dr. Diane Mueller, I am now happy to say I have more consciousness surrounding how I eat, what to eat and when things are appropriate. Living by example Dr. Mueller has a vibrancy that makes you want to learn and know more about your body and overall health. I highly recommend her to anyone looking for new answers, a new approach to health, or in need of freedom from pain and limitations.”
-Storie S.
Kihei, HI
