
Written by Dr. Diane Mueller
What does a positive IgM Lyme test mean? It can mean your immune system recently reacted to Borrelia burgdorferi, the bacteria linked to Lyme disease. But it does not automatically prove you have an active Lyme infection.
That gap between “positive” and “clear answer” is where many patients get stuck. I’ve seen this again and again in people with fatigue, joint pain, brain fog, headaches, and strange neurologic symptoms who were told opposite things by different doctors. One says, “You definitely have Lyme.” Another says, “Ignore it, it’s a false positive.” Neither answer helps if you still feel awful.
The truth is more specific. IgM is an early antibody. It tends to matter most in the first few weeks after infection. After that, the result gets much harder to interpret on its own. And if you live in or near high-risk areas like Fairfield County or spend time around wooded parts of Connecticut, exposure history matters more than people think.
In this guide, I’ll explain what a positive IgM Lyme test means, when it may matter, when it may mislead you, and what to do next so you stop guessing and start getting real answers.
A positive IgM Lyme test indicates a recent immune response to Borrelia burgdorferi, typically within 30 days of symptom onset, but does not confirm active Lyme disease alone.
Timing, symptoms, and exposure history in Lyme-endemic areas are crucial to accurately interpret a positive IgM Lyme test and guide further diagnosis.
Isolated IgM positivity beyond 30 days without IgG antibodies is often unreliable and may represent a false positive or incomplete testing.
Always obtain the full lab report including test type and IgG results to better understand your Lyme test and decide if follow-up testing is needed.
Consider broader health evaluations for persistent symptoms, as other infections, mold exposure, or immune conditions can mimic or overlap with Lyme disease symptoms.
A thorough symptom and exposure timeline combined with comprehensive clinical evaluation helps move from test confusion to clear, actionable diagnosis and treatment.
We have helped thousands of people in Colorado, Wyoming, New Jersey, Pennsylvania, Texas, Wisconsin restore their health and quality of life by diagnosing and treating their Lyme Disease.
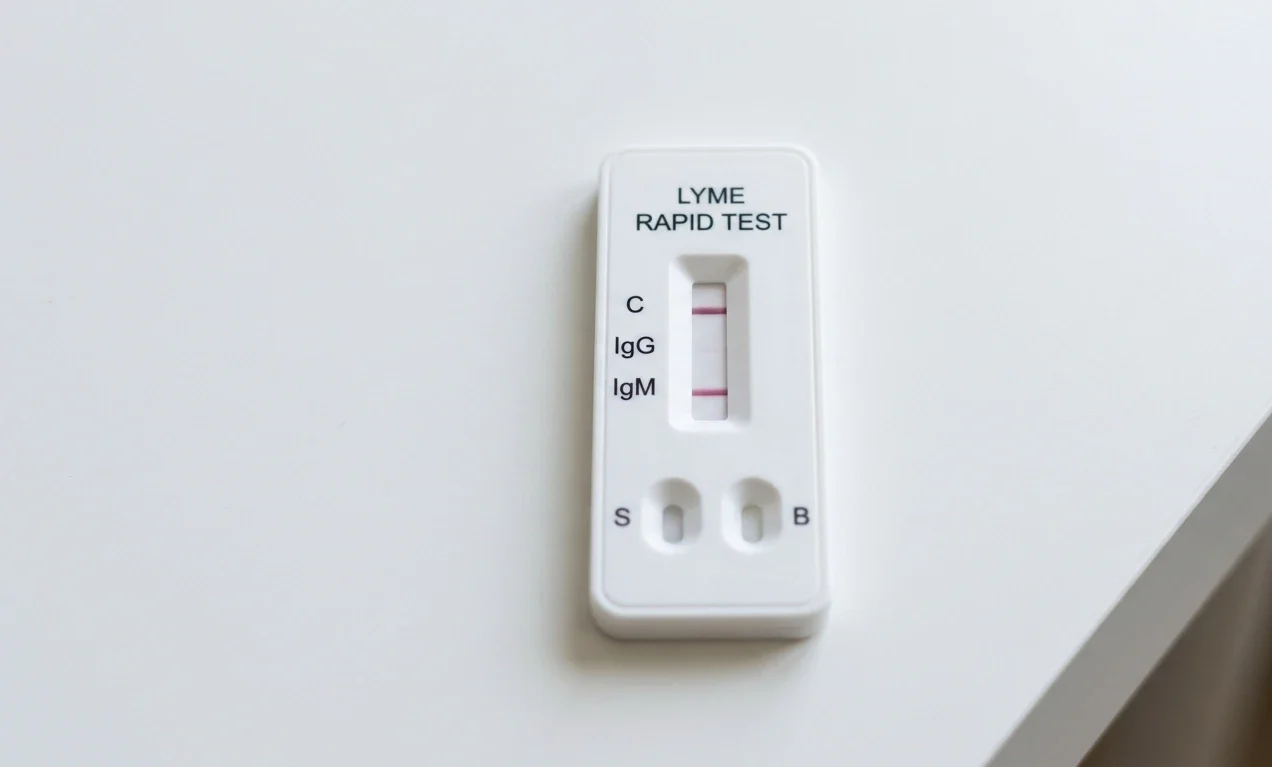
A positive IgM Lyme result causes confusion because it sits in a gray zone. It can point to early infection, or it can be misleading. Both things are true.
Many patients assume any positive Lyme marker equals a firm diagnosis. That would be simpler. It’s just not how Lyme testing works. The Centers for Disease Control and Prevention (CDC) and other experts note that IgM results are most useful within 30 days of symptom onset. After that window, isolated IgM positivity becomes much less reliable.[1][3]
IgM antibodies are your body’s first wave immune response. They usually start to appear about 1 to 2 weeks after infection. Later, the immune system typically shifts toward IgG antibodies, which reflect a more mature immune response.[3][5]
Think of IgM as the smoke alarm that goes off first. It may alert you early, but it does not tell the full story by itself.
If you had a recent tick bite, a new rash, fever, body aches, or sudden joint pain in the last few weeks, a positive IgM may fit that picture. In that setting, the result can be meaningful.
Action step: Write down the exact date your symptoms started and any known tick exposure. Do this today. It takes 10 minutes and makes your test much easier to interpret.
A positive result does not always mean active Lyme disease because IgM tests can produce false positives. Other infections, immune activity, and even test method differences can trigger confusing results.[1][3][6]
This is where patients often feel dismissed. You finally get a “positive” lab, and then someone tells you it means nothing. That feels awful. But the real issue is not that your symptoms are imaginary. The issue is that one lab marker cannot carry the whole diagnosis.
If your only abnormal result is an isolated IgM positive months after symptoms began, that result needs caution. The CDC advises clinicians not to rely on IgM alone beyond 30 days because true Lyme cases should usually show IgG by then.[1][3]
Action step: Ask for a copy of the full report, not just the word “positive.” You need the test type, bands, and whether IgG was also checked.
The fastest way to interpret a positive IgM Lyme test is this: timing matters most. The same result means different things at day 14 than it does at month 6.
IgM positivity may reflect a recent immune response if symptoms began less than 30 days ago. This is the setting where IgM has the most clinical value.[3]
Examples include:
A known tick bite 2 to 4 weeks ago
A new bull’s-eye rash
Sudden flu-like symptoms during tick season
New joint pain, fever, or headache after outdoor exposure
In places with meaningful Lyme exposure, including many parts of Connecticut and nearby New England regions, that pattern raises the pre-test probability. If you hiked near wooded trails, worked in brush, or spent time in backyards near stone walls and deer traffic, your exposure history counts.
If you have IgM positive and IgG negative within the first month, that can support early Lyme. It still needs symptom and exposure review, but it is more believable in that early window.[3][7]
Action step: Build a simple timeline with three columns: symptom start, tick exposure, and testing date. This takes 15 minutes and often changes the conversation.
A positive IgM can be misleading when symptoms have been present more than 30 days and IgG is still negative. In that case, isolated IgM often points to a false positive, incomplete testing, or another process entirely.[1][3]
This is one of the hardest parts emotionally. You may have been sick for months or years. You want a clean answer. But an isolated IgM does not reliably prove chronic Lyme.
It also does not prove you are fine. That distinction matters.
I’ve seen patients arrive after spending thousands of dollars chasing one old IgM result while untreated mold exposure, Epstein-Barr virus reactivation, thyroid dysfunction, or Bartonella symptoms kept driving the illness. The lab was not useless. It was just not the whole map.
Action step: If your symptoms are long-standing, do not anchor on one IgM result. Ask what else has been ruled in or ruled out.
Symptoms, exposure history, and timing still matter because Lyme remains a clinical diagnosis supported by testing, not replaced by testing.[2][3]
A positive test means more when it matches:
Tick exposure in a Lyme-endemic area
Symptoms that fit Lyme disease
Testing done in the right time window
Confirmatory methods such as standard two-tier testing
A positive test means less when there is no exposure history, symptoms started long ago, or the testing method is unclear.
This is why two people can hold the same lab printout and need completely different next steps. A runner in Greenwich with a summer tick bite and new fever is not the same case as someone with five years of fatigue and one isolated IgM band.
Action step: Bring your symptom list, exposure history, and full lab report to your next appointment. Keep it to one page so your clinician can see the pattern fast.
We have helped thousands of people in Colorado, Wyoming, New Jersey, Pennsylvania, Texas, Wisconsin restore their health and quality of life by diagnosing and treating their Lyme Disease.
False positive or unclear IgM results happen more often than most patients are told. That does not mean the test is worthless. It means the result must be placed in context.
Cross-reactivity means antibodies made for one infection react with parts of another test. This can create a Lyme result that looks positive when Lyme is not the true cause.[6]
Examples can include:
Viral infections such as Epstein-Barr virus
Other bacterial infections
Autoimmune activity
Non-specific immune activation
Some Lyme bands are more specific than others. Others can light up for less specific reasons. That is one reason a full interpretation matters more than a simple yes-or-no summary.
Action step: Ask whether your clinician reviewed possible cross-reactivity, especially if you had a recent virus, autoimmune markers, or an unusual symptom pattern.
Testing too early can produce confusing results because your body may not have made enough antibodies yet. Testing without enough clinical context can also inflate false positives, especially in low-risk situations.[3]
Here’s the practical problem:
Very early testing can miss Lyme because antibodies have not risen yet
Late isolated IgM positivity can mislead because IgG should usually appear by then
Testing people with very low exposure risk lowers the chance that a positive result reflects true Lyme
So yes, timing can cut both ways. Too soon is a problem. Too late with only IgM is also a problem.
Action step: If testing was done very early, ask whether repeat testing was recommended based on symptom timing.
Lab method matters. Not all Lyme tests are interpreted the same way. Standard CDC-recommended testing usually involves a two-step process, such as an enzyme immunoassay followed by an immunoblot or another approved confirmatory method.[1][8]
For IgM immunoblots, the classic criteria require 2 of 3 significant bands for a positive result. Some specialty labs use different methods or expanded criteria. That can offer useful clues in some cases, but it can also create confusion if patients do not know exactly what was measured.
This is where details matter: Was it an ELISA? A Western blot? Modified two-tier testing? A specialty panel? If you tested in Stamford, then reviewed results with another doctor in Boston, those clinicians may not be speaking from the same testing framework.
Action step: Call the lab or portal today and get the exact test name, date, and interpretation method. Save a PDF copy.

After a positive IgM Lyme test, do not panic and do not ignore it. Organize the facts first. That step alone can prevent months of confusion.
Start with a simple timeline. When did symptoms begin? When might exposure have happened? When was the test drawn?
Include details such as:
Tick bite or rash date
Outdoor exposure location
First day of fever, fatigue, pain, or brain fog
Date antibiotics started, if any
Date each Lyme test was run
This sounds basic, but it is often the missing piece. A clean timeline can show whether IgM fits an early infection window or looks out of place.
Action step: Use your phone notes app and make the timeline in 20 minutes.
Next, confirm the exact test. Was it a screening EIA, a Western blot, or a full two-tier test? Was IgG also measured? If not, you may need follow-up testing, depending on your symptom timing and clinical picture.[1][6]
Questions to ask:
Was this CDC-standard two-tier testing?
Was IgG negative, positive, or not done?
Were enough IgM bands present for a true positive?
Was testing done before 30 days or after?
Should testing be repeated or expanded?
This is especially important if your result came from a quick summary line in a portal. “Positive” without method details is not enough.
Action step: Send a portal message with those five questions today. It usually takes less than 10 minutes.
One lab marker should never outrank the full story. The bigger clinical picture includes symptoms, exposures, response to prior treatment, coinfections, mold history, immune function, and other root causes.
This matters most for people with chronic symptoms. If you have crushing fatigue, air hunger, night sweats, sensory changes, sinus issues, or flares after water-damaged buildings, Lyme may be only one layer of the case. On mylymedoc.com, this is the core clinical lens: stop guessing and look at the full pattern.
For patients who feel failed by conventional care, this broader workup often brings the first real sense of direction.
Action step: Make a one-page health summary with your top 10 symptoms, major exposures, old labs, and treatment history before your next visit.
Sometimes Lyme is part of the picture. Sometimes it is not. And sometimes Lyme, mold, and other infections overlap so closely that one positive IgM result distracts from the bigger problem.
Coinfections and mold exposure can create symptoms that look a lot like Lyme disease. Fatigue, joint pain, dizziness, headaches, sleep disruption, anxiety, histamine issues, and brain fog can appear in all of them.
Common overlapping issues include:
Mold exposure from water-damaged buildings
Thyroid dysfunction
Gut imbalance
Nervous system dysregulation
Reactivated viruses
I’ve seen patients focus hard on one Lyme marker while ignoring the musty basement smell at home, the office leak above their desk, or the symptom flare every time they enter a damp building. Those details matter. They are not random.
Action step: List all possible exposures from the last 12 months, including home, work, travel, pets, and water-damaged spaces.
Persistent symptoms deserve a broader workup because long-term illness rarely stays confined to one system. If symptoms continue even though treatment, or if Lyme testing is mixed and unclear, a wider evaluation can prevent missed diagnoses.[6]
A stronger workup may include review of:
Lyme and coinfection testing history
Mold and mycotoxin exposure history
Thyroid markers
Iron, B12, and vitamin D status
Inflammatory markers
Gut symptoms and stool testing when relevant
Nervous system and sleep pattern changes
This does not mean every patient needs every test. It means the workup should match the pattern. If you live in Connecticut, spend time in wooded areas, and also react strongly to damp buildings, both Lyme and mold need serious consideration.
Action step: If you have symptoms lasting more than 6 to 8 weeks, ask for a broader root-cause review instead of repeating the same basic Lyme test alone.
We have helped thousands of people in Colorado, Wyoming, New Jersey, Pennsylvania, Texas, Wisconsin restore their health and quality of life by diagnosing and treating their Lyme Disease.
A positive IgM Lyme test means your immune system showed an early-type antibody response, but the result only becomes useful when matched with timing, symptoms, exposure history, and the right testing method.
If symptoms started within the last 30 days, IgM may support early Lyme. If symptoms are older and IgG is still negative, isolated IgM is much more likely to be unclear or false positive.[1][3]
Most important, do not let one lab result define your entire case. If you still feel sick, you deserve a clinician who will look at the whole picture and fight for real answers.
Start here today:
Build your symptom and exposure timeline
Get the full lab report
Confirm the test method
Review whether IgG and follow-up testing were done
Ask whether coinfections, mold, or other root causes fit your pattern
That is how you move from confusion to clarity. Not by guessing. By putting the pieces in the right order.
A positive IgM Lyme test shows your immune system has recently reacted to Borrelia burgdorferi, usually within 30 days of infection. It suggests early Lyme disease but needs clinical context to confirm, as IgM can produce false positives.
No, a positive IgM test alone does not confirm active Lyme disease, especially if symptoms started more than 30 days ago. IgG antibodies typically become positive later, so isolated IgM results after a month may be false positives or unrelated to Lyme infection.
Timing is critical; IgM antibodies usually appear 1–2 weeks after infection and are most reliable within 30 days of symptom onset. After 30 days, IgM positivity without IgG is less reliable and often misleading in diagnosing Lyme disease.
False positives in IgM Lyme testing often result from cross-reactivity with antibodies from other infections like Epstein-Barr virus, autoimmune activity, or lab testing variability. This means IgM alone can’t reliably diagnose Lyme disease without clinical correlation.
After a positive IgM test, review your symptom onset and tick exposure timeline, obtain the full lab report including test type and IgG status, consult your healthcare provider for appropriate follow-up testing, and consider broader evaluations if symptoms persist.
Yes, symptoms similar to Lyme disease can be caused by coinfections like Bartonella, mold exposure, thyroid dysfunction, or viral reactivations. A comprehensive medical evaluation is important to identify all potential causes.
Sources: CDC Lyme testing guidance: peer-reviewed reviews on Lyme serology and two-tier testing.[1][2][3][5][6][7][8]
We have helped thousands of
people restore their health
and quality of life by diagnosing
and treating their Lyme Disease.
“Dr. Mueller’s approach to medicine is refreshing! There is only so much you can do with western medicine and in my life I was needing a new approach. By addressing the whole body, nutritional diet factors, environmental factors, blood work, and incorporating ideas I had not previously known, I was able to break through with my conditions. I am not only experiencing less pain in my life, but through the process of healing guided by Dr. Diane Mueller, I am now happy to say I have more consciousness surrounding how I eat, what to eat and when things are appropriate. Living by example Dr. Mueller has a vibrancy that makes you want to learn and know more about your body and overall health. I highly recommend her to anyone looking for new answers, a new approach to health, or in need of freedom from pain and limitations.”
-Storie S.
Kihei, HI
