
Written by Dr. Diane Mueller
One of the most common things I hear is, “I treated Lyme… so why do I still feel like my body is on fire?” And honestly, that question makes sense. You do the antibiotics, clean up your diet, buy the supplements, spend way too much money on things with labels you can’t pronounce, and yet you’re still dealing with anxiety, foot pain, weird rashes, heart flutters, or a brain that feels like it’s buffering.
That’s where Bartonella enters the conversation.
Bartonella symptoms can be sneaky, intense, and oddly specific at the same time. They often get brushed off as stress, “just inflammation,” or plain bad luck. But if you’ve been dealing with chronic illness, suspected Lyme, or stubborn symptoms after treatment, this pattern matters. A lot.
And no, you’re not imagining it.
In clinical practice, Bartonella signs and symptoms often show up in clusters, neurological, vascular, skin, psychiatric, and pain-related. The tricky part is that they can overlap with Lyme, Babesia, mold illness, even autoimmune conditions. It can feel like one of those detective shows where every clue points in three directions at once.
So let’s slow it down and sort the signal from the noise. You’ll get a practical, root-cause view of bartonella symptoms in humans, how they differ from Lyme, why chronic cases can drag on, and what proper testing and treatment usually require when standard care hasn’t been enough.
Bartonella symptoms often overlap with Lyme disease but are characterized by sharp nerve pain, specific psychiatric changes, foot and shin pain, vascular issues, and distinctive stretch-mark-like rashes.
Neurological symptoms such as brain fog, insomnia, mood swings, and sensory sensitivity are hallmark signs of Bartonella infection and should not be dismissed as psychological.
Diagnosis of Bartonella requires careful clinical history, physical examination, and targeted testing since standard labs can miss chronic or complex cases.
Effective Bartonella treatment involves a personalized, multi-faceted approach including antimicrobial therapy, detox support, nervous system regulation, and care for co-infections like Lyme and Babesia.
Persistent Bartonella symptoms after treatment are common due to immune evasion, incomplete therapy, and overlapping conditions, making specialist care essential for proper management.
Recognizing Bartonella symptom clusters and seeking a specialist familiar with co-infections improves diagnosis accuracy and treatment outcomes significantly.
We have helped thousands of people in Colorado, Wyoming, New Jersey, Pennsylvania, Texas, Wisconsin restore their health and quality of life by diagnosing and treating their Lyme Disease.
Bartonella is a group of bacteria that can infect humans and affect the blood vessels, nervous system, immune system, skin, and connective tissue. The species people talk about most often is Bartonella henselae, which is classically linked to cat scratch disease symptoms. But in chronic illness practice, the story is often bigger than a cat scratch.
You can be exposed through scratches, bites, fleas, lice, sand flies, and possibly ticks. That’s one reason people asking how do you get bartonella often get frustrated, the transmission story isn’t always neat and obvious.
In acute cases, Bartonella may cause swollen lymph nodes, fever, and fatigue. In more complex or chronic cases, bartonella disease symptoms can become far more systemic:
nerve irritation
mood changes
burning soles or shin pain
unusual stretch-mark-like rashes
vascular inflammation
sleep disruption
Some mainstream summaries, including what bartonellosis can look like clinically, focus on short-term infection. That’s useful, but it often misses the patients who still feel unwell months later.
That’s where a functional, Lyme-literate lens matters. In the real world, Bartonella rarely travels alone. It commonly overlaps with Lyme, Babesia, mold toxicity, gut dysfunction, and nervous system dysregulation. Sequence matters. If you treat one layer and ignore the rest, symptoms can keep circling back like an unwelcome houseguest who never takes the hint.
If there’s one place Bartonella tends to make itself known, it’s the nervous system. Bartonella neurological symptoms often feel sharp, wired, and uncomfortable rather than just “tired and achy.” Patients describe internal buzzing, agitation, burning pain, sensory sensitivity, tremors, headaches, dizziness, and episodes of sudden panic that seem to come out of nowhere.
You may also notice:
brain fog that feels electrically scrambled
insomnia, especially waking around 2-4 a.m.
light and sound sensitivity
tingling, numbness, or nerve pain
mood swings, irritability, rage, or anxiety
This is also why bartonella psychiatric symptoms get missed. They’re real. They’re not “all in your head.” Bartonella can affect neuroinflammation, vascular function, and the autonomic nervous system. That can create a body that feels stuck in fight-or-flight.
Clinically, I pay attention when someone says, “I don’t feel like myself anymore.” That sentence carries weight.
If your picture is especially confusing, neurological symptoms can overlap between Lyme and Bartonella in ways that muddy the waters fast. And in mixed infections, the symptom burden often climbs.
We have helped thousands of people in Colorado, Wyoming, New Jersey, Pennsylvania, Texas, Wisconsin restore their health and quality of life by diagnosing and treating their Lyme Disease.
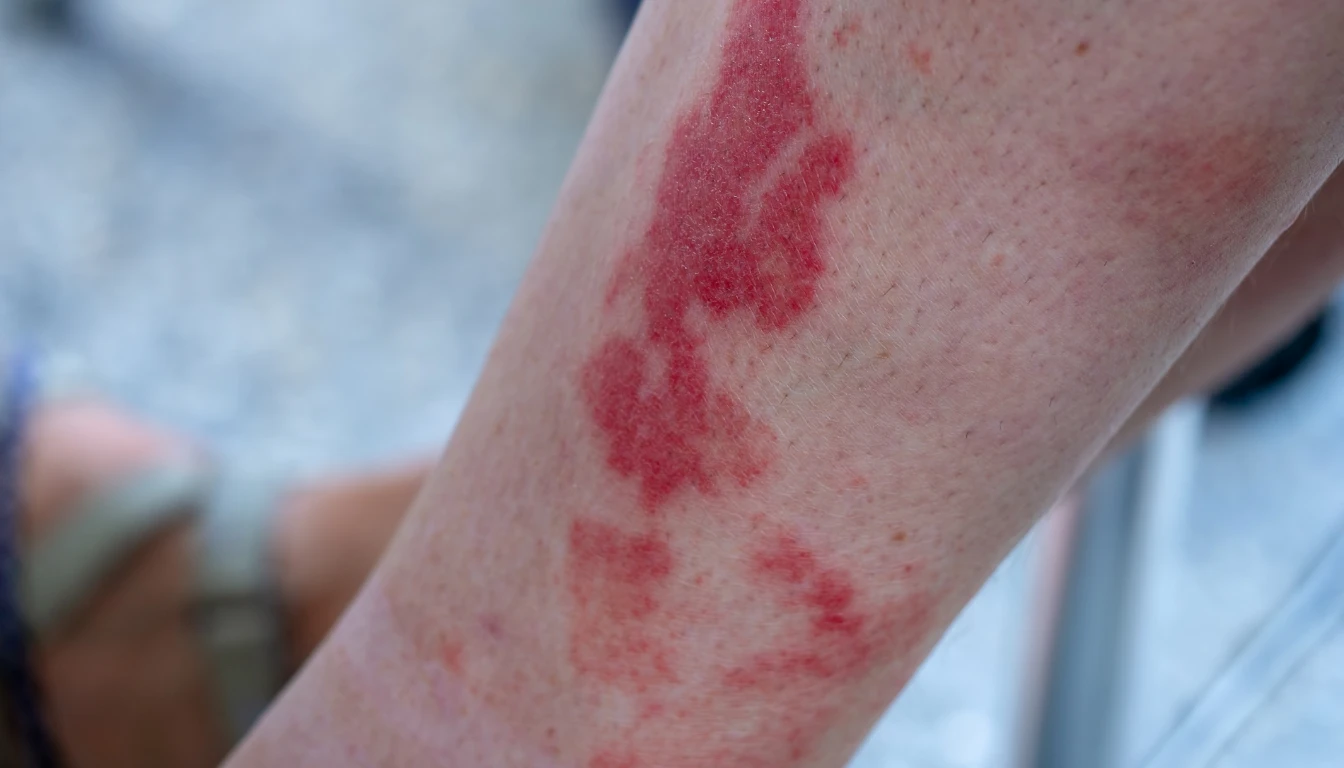
The skin clues can be surprisingly specific. Bartonella rash symptoms often include red, purple, or pink linear streaks that look like stretch marks, but they may appear in places where ordinary stretch marks don’t make much sense, like the back, hips, arms, or torso without major weight change. People often call these bartonella stretch marks.
They can look:
rippled or streaky
reddish at first, then darker
like scratches under the skin
tender or completely painless
Not every person gets them. But when they show up with neurological symptoms, foot pain, and psychiatric changes, they’re a major clue.
You may also see flushing, mottled skin, easy bruising, visible capillaries, or slow wound healing. Bartonella has a vascular component, so skin changes aren’t just cosmetic, they can reflect deeper inflammation in blood vessels and connective tissue.
One patient once told me her rash looked like “I lost a fight with a tiger, except I hadn’t left the couch.” Oddly funny, yes. Also very clinically useful.
Bartonella can irritate the vascular system in ways that feel scary, especially if nobody has explained the pattern. Common bartonella signs and symptoms here include heart palpitations, chest discomfort, shortness of breath, dizziness on standing, cold hands and feet, and a sense that your circulation is just… off.
Some people also develop:
POTS-like symptoms
blood pressure swings
headaches from vascular irritation
visible veins or capillary fragility
air hunger when co-infections are present
This doesn’t always mean structural heart disease. But it does mean your symptoms deserve a serious look.
Bartonella can drive endothelial inflammation, the lining of the blood vessels gets irritated, and that can create widespread issues from poor temperature regulation to pounding heartbeats. In patients with bartonella co-infection symptoms, I often see the vascular piece mixed with neuropsychiatric symptoms and pain.
When you’re trying to sort out overlaps, see our full comparison of Lyme, Bartonella, and Babesia because Babesia can add air hunger and sweats, while Bartonella often adds the sharper nerve-and-vessel pattern.
GI symptoms don’t get enough attention in Bartonella discussions. But they should. You may have nausea, abdominal pain, reduced appetite, reflux, bloating, constipation, loose stools, or a stomach that becomes dramatically more reactive during flares.
Part of this is immune activation. Part may be nervous system dysfunction, when your autonomic system is stressed, digestion often slows down or gets chaotic. And part of it is overlap. Bartonella rarely appears in a perfectly isolated box.
In chronic cases, people sometimes notice that their gut symptoms worsen alongside anxiety, insomnia, or pain spikes. That’s not random. It’s one interconnected circuit.
A simple way to picture it: when the body senses threat, digestion moves to the back seat. It’s hard to run “rest and digest” when your system is flooring the gas pedal.
This is where bartonella functional medicine approaches can help, because treatment often has to include microbiome support, inflammation control, refresh pathways, and nervous system regulation, not just antimicrobials alone.
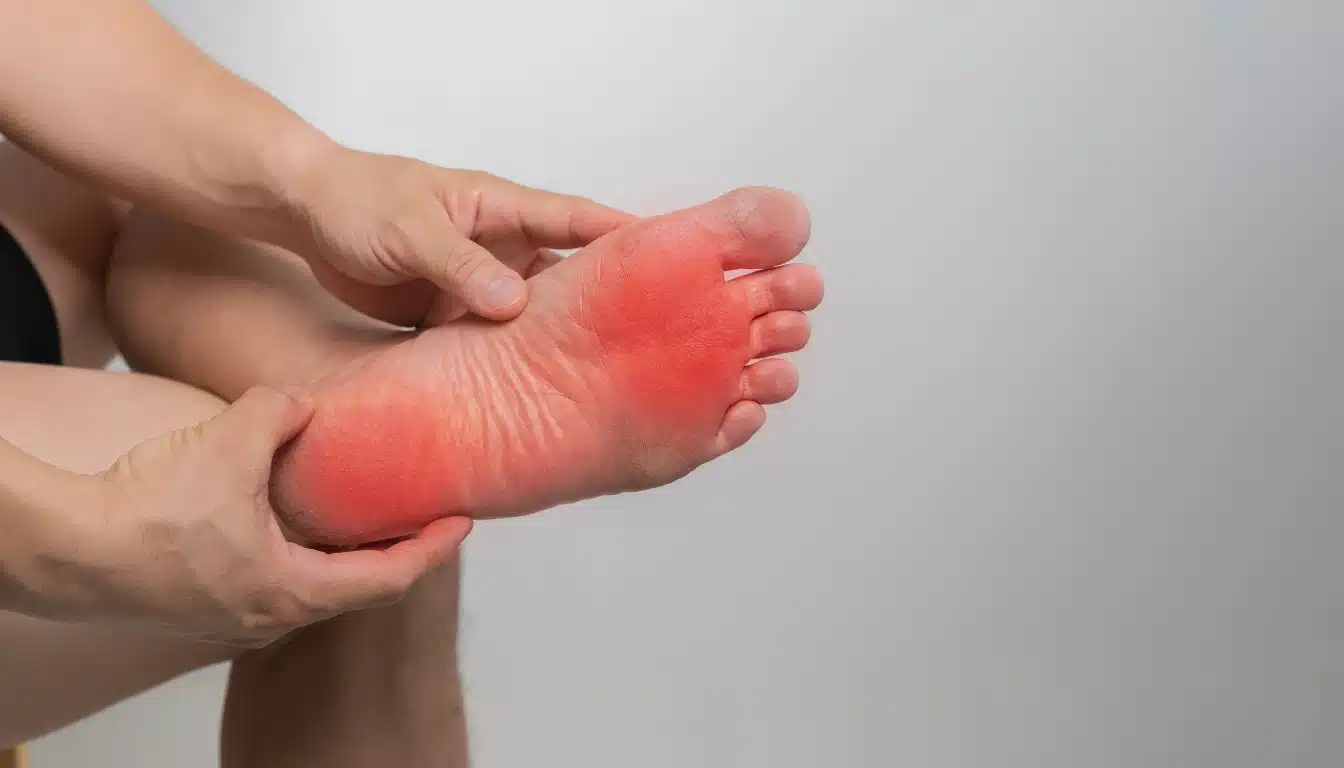
Some of the most classic symptoms of bartonella are pain-based. And not always the standard “deep joint pain” people associate with Lyme. Bartonella often causes sharper, more focal discomfort.
Common patterns include:
sore soles, especially first thing in the morning
shin pain or tenderness
migrating muscle pain
rib pain or chest wall soreness
jaw tension and neck tightness
tendon or fascia irritation
That foot pain clue matters. A lot of patients mention stepping out of bed and feeling like they’re walking on bruises, thumbtacks, or hot gravel. Not elegant language, but very memorable.
Bartonella can affect connective tissue, blood vessels, and nerves, which helps explain why the pain can feel both inflammatory and neuropathic. It may move. It may flare without obvious reason. It may worsen with stress or Herx reactions.
If Lyme is also in the picture, Bartonella and Lyme co-infections together can create a much more intense pain and neuroinflammatory picture than either infection alone.
Then there’s the whole-body layer: fatigue, fevers, swollen glands, chills, night sweats, chemical sensitivity, weakness, poor stress tolerance, and that flu-ish “I’m sick but nothing is showing up clearly” feeling.
These bartonella symptoms in humans can be easy to dismiss because they overlap with so many other conditions. But the pattern matters more than any single symptom.
You may notice flares after:
lack of sleep
emotional stress
travel
mold exposure
overexertion
starting treatment too aggressively
That last one is a big deal. When microbial load, inflammation, and refresh strain all collide, the body can push back hard.
And with bartonella henselae symptoms, the presentation can range from mild and localized to chronic and multisystem. Some patients start with swollen lymph nodes and fever: others never remember an acute phase at all.
If your symptom picture keeps shifting, a side-by-side tool helps. You can use our co-infections symptom comparison chart when you’re trying to organize what’s Bartonella-like versus what sounds more like Lyme or Babesia.
This is one of the biggest points of confusion online, and fair enough, the overlap is real. Bartonella vs lyme symptoms are not always cleanly separated. But some patterns show up often enough to guide the conversation.
Bartonella tends to lean more toward:
burning or sharp nerve pain
psychiatric or mood symptoms
rage, panic, agitation
foot pain and shin pain
vascular issues and odd rashes
stretch-mark-like skin lesions
Lyme often leans more toward:
migrating joint pain
fatigue and flu-like symptoms
cognitive slowing
facial palsy in some cases
broader multisystem fluctuation
That said, this isn’t a neat little chart in real life. Many patients have bartonella lyme disease overlap, and that can produce a blended picture of anxiety, neuropathy, joint pain, brain fog, insomnia, palpitations, and fatigue.
One practical clue: if your symptoms feel intensely neurological, psychiatric, vascular, or pain-in-the-soles specific, Bartonella deserves strong consideration.
It’s less about naming one villain and more about recognizing the whole cast.
We have helped thousands of people in Colorado, Wyoming, New Jersey, Pennsylvania, Texas, Wisconsin restore their health and quality of life by diagnosing and treating their Lyme Disease.
This is the part that leaves people discouraged. You took treatment. Maybe you even improved for a while. Then symptoms came back, or never fully left.
Chronic bartonella symptoms can persist for several reasons.
First, Bartonella is good at immune evasion. It can hide in cells and affect tissues that are harder to fully clear. Second, treatment is often incomplete or poorly matched to the infection burden. Third, co-infections, mold exposure, gut dysfunction, nervous system stress, and refresh problems can keep the body inflamed even after some microbial load drops.
There’s also the issue of persistence biology. If you’ve already gone down the Lyme rabbit hole at 1 a.m., you’ve probably heard of biofilms and hard-to-eradicate microbial states. That framework matters here too, especially when considering persister cells’ role in Lyme disease. Persistent symptoms aren’t always “ongoing infection only,” but they also shouldn’t be dismissed as imaginary or irrelevant.
I’ve seen people stall because treatment started too hard, too fast, without enough support for drainage, gut health, sleep, or mast cell reactivity. Others plateau because Lyme gets treated while Bartonella is missed.
This is why order matters. If the terrain is inflamed and the roadmap is messy, even good tools can underperform.
Bartonella diagnosis is part science, part pattern recognition, and yes, sometimes part frustration. Standard labs can miss it. A negative test does not always rule it out, especially in chronic, deep-funnel cases where symptoms have been evolving for months or years.
Diagnosis usually involves three buckets:
Your timeline matters. Exposure history, symptom pattern, response to prior treatment, psychiatric changes, foot pain, vascular signs, and unusual rashes all matter.
A practitioner may look for skin lesions, lymph node changes, vascular patterns, temperature dysregulation, and neurological findings.
Testing may include serology, PCR, specialty labs, inflammatory markers, and broader co-infection workups. But Bartonella is notorious for inconsistent detectability, so the best clinicians use testing as one tool, not the whole truth.
If you’re sorting through options, these co-infection testing options can help frame what questions to bring to your appointment.
A quick reality check: good diagnosis is rarely about one magic lab. It’s about symptom clusters, differential diagnosis, and ruling in or out the other root-cause pieces, Lyme, Babesia, mold, MCAS, gut issues, thyroid, nutrient depletion, all of it. That can feel like a lot. It is a lot. But it’s also how you stop guessing.

Proper Bartonella treatment is rarely a one-pill, one-week situation. If you’ve been searching for a simple answer, I get it. Everyone wants the clean movie ending. Real chronic infection care is usually more like renovating an old house, you fix wiring, plumbing, and the leak in the ceiling, not just the paint.
Treatment often requires a combination of:
antimicrobial therapy, sometimes in rotation or combination
support for detoxification and drainage
gut and liver protection
nervous system regulation
anti-inflammatory and mast-cell-aware strategies
treatment of overlapping Lyme, Babesia, or mold issues
That’s why discussions about co-infection treatment options matter so much. In some cases, medications like rifampin for Lyme and Bartonella or a rifabutin protocol may be part of the conversation, depending on your history, tolerance, and broader clinical picture.
But meds alone are not the whole protocol.
You need sequencing. If your nervous system is fried, your gut is inflamed, and your refresh capacity is overwhelmed, aggressive treatment can backfire. The best outcomes usually come from a personalized plan that respects your symptom intensity, your financial reality, and your body’s actual capacity to heal.
Bartonella is one of those infections that exposes the limits of rushed medicine. A quick urgent-care visit may catch acute cat scratch disease. But chronic Bartonella? With psychiatric symptoms, mold overlap, Lyme history, Herx reactions, and a stack of “normal” labs? That takes a specialist eye.
You need someone who can:
recognize symptom patterns across systems
distinguish Bartonella from Lyme, Babesia, mold, and autoimmune lookalikes
understand test limitations
build a phased treatment plan
adjust treatment when your body reacts strongly
This matters emotionally, too. If you’ve been told your symptoms are anxiety, overwork, or “just stress,” you may already be carrying medical trauma. Being believed is not a luxury. It changes compliance, hope, and outcomes.
The right clinician won’t promise magic. They’ll give you a roadmap. They’ll explain why sequence matters, what to watch, and when to pivot.
If you’re at the stage where self-research has become a second job, finding the right specialist can save you time, money, and a lot of expensive headaches down the road.
And if you want direct support, you can work with Dr. Diane through a Lyme-literate, root-cause approach built for complex chronic cases.
If this symptom picture felt uncomfortably familiar, trust that signal. Bartonella symptoms often hide in plain sight, inside anxiety that doesn’t feel psychological, pain that migrates strangely, stretch-mark-like rashes, foot pain, palpitations, insomnia, and a nervous system that won’t fully settle down.
You do not need to keep white-knuckling your way through confusing symptoms while being told everything looks fine.
The goal isn’t to label every sensation with perfect certainty on day one. The goal is to recognize patterns, rule out overlap, and build a treatment sequence that actually fits your body. That’s how people stop spinning in circles.
If you’re ready for real answers and a clearer next step, you can get treatment with a team that understands Lyme, Bartonella, co-infections, and the root-cause layers that so often get missed. Healing gets a lot more possible when the roadmap finally makes sense.
Medical disclaimer: This article is for education only and is not a substitute for personal medical care, diagnosis, or emergency treatment.
We have helped thousands of people in Colorado, Wyoming, New Jersey, Pennsylvania, Texas, Wisconsin restore their health and quality of life by diagnosing and treating their Lyme Disease.
Yes. Bartonella is its own infection transmitted by fleas, lice, and sand flies, not just ticks. However, patients who were bitten by a tick may have acquired both Lyme and Bartonella simultaneously, as ticks can carry multiple co-infections.
In immunocompetent people, cat scratch disease (the acute form) often resolves. However, in the chronic form, particularly in patients with Lyme or immune compromise, Bartonella does not resolve without treatment
It’s real, and it’s physiological. Bartonella directly infects the nervous system and produces neuroinflammation that manifests as anxiety, panic, and rage disproportionate to circumstances. This is one of the most distressing symptoms of Bartonella because it makes patients question their mental health — when in fact it’s an infectious neurological symptom.
Bartonella can produce two distinct skin findings: (1) stretch mark-like striae that appear without weight gain, often on the abdomen, flanks, or inner thighs; and (2) linear red streaks that follow lines of skin tension. Neither looks like the Lyme bullseye rash.
Untreated or inadequately treated chronic Bartonella can cause persistent neurological damage, vascular complications, and prolonged immune dysfunction. With proper treatment including adequate support for the nervous system, most patients improve significantly.
Seek medical care promptly if you have an engorged tick, a spreading rash, flu-like symptoms after a bite, or warning signs such as severe headache, neck stiffness, shortness of breath, fainting, facial droop, chest pain, or palpitations. Tick testing is not a diagnosis, so do not delay care while waiting on results.
Schaller, J. L., Burkland, G. A., & Langhoff, P. J. (2007). Do Bartonella infections cause agitation, panic disorder, and treatment-resistant depression? Medscape General Medicine, 9(3), 54. https://pmc.ncbi.nlm.nih.gov/articles/PMC2100128/
Mada, P. K., & Castano, G. (2023). Bartonellosis. In StatPearls. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK430874/
Allizond, V., et al. (2019). Serological and molecular detection of Bartonella henselae in specimens from patients with suspected cat scratch disease in Italy: A comparative study. PLOS ONE. https://pmc.ncbi.nlm.nih.gov/articles/PMC6368319/
We have helped thousands of
people restore their health
and quality of life by diagnosing
and treating their Lyme Disease.
“Dr. Mueller’s approach to medicine is refreshing! There is only so much you can do with western medicine and in my life I was needing a new approach. By addressing the whole body, nutritional diet factors, environmental factors, blood work, and incorporating ideas I had not previously known, I was able to break through with my conditions. I am not only experiencing less pain in my life, but through the process of healing guided by Dr. Diane Mueller, I am now happy to say I have more consciousness surrounding how I eat, what to eat and when things are appropriate. Living by example Dr. Mueller has a vibrancy that makes you want to learn and know more about your body and overall health. I highly recommend her to anyone looking for new answers, a new approach to health, or in need of freedom from pain and limitations.”
-Storie S.
Kihei, HI
